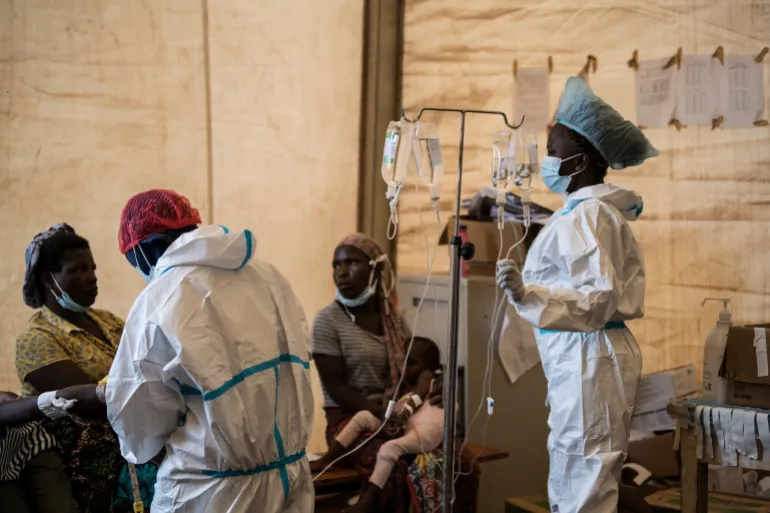
The Nigeria Centre for Disease Control and Prevention (NCDC) has issued a warning about the rising trend of cholera cases across the country as the rainy season intensifies.
In a statement signed by its Director General, Dr Jide Idris, the NCDC reported that from 1 January to 11 June, 2024, there have been 1,141 suspected and 65 confirmed cases of cholera, resulting in 30 deaths from 96 Local Government Areas (LGAs) across 30 states.
The NCDC highlighted that ten states—Bayelsa, Zamfara, Abia, Cross River, Bauchi, Delta, Katsina, Imo, Nasarawa, and Lagos—account for 90 per cent of the cholera burden.
It, however, stated that a multi-sectoral National Cholera Technical Working Group, led by the centre and comprising the Federal Ministries of Environment and Water Resources, the National Primary Health Care Development Agency, the World Health Organization, the United Nations Children’s Fund, and other partners, has been providing support to the affected states.
“This support includes risk communication, active case search, laboratory diagnosis, case management, provision of response commodities, water sanitation and hygiene interventions, and dissemination of Cholera awareness jingles in English and local languages,” it said.
Cholera
Cholera is a food and water-borne disease caused by the ingestion of the bacterium Vibrio cholerae through contaminated water and food, typically tainted by the feces of infected individuals.
It frequently occurs in countries like Nigeria, where access to clean drinking water and adequate sanitation is limited.
Although cholera is both preventable and treatable, the incidence of the disease tends to rise with the onset of the rainy season.
The NCDC noted that beverages prepared with contaminated water, such as those sold by street vendors, as well as ice and even commercial bottled water, have been implicated in the transmission of cholera.
“The time between infection and the appearance of symptoms is two hours to five days. It has a higher risk of transmission in areas that lack adequate sanitation facilities and a regular supply of clean water.
“Unsafe practices such as improper disposal of refuse and open defecation endanger the safety of water used for drinking and personal use,”.
The infectious disease agency said symptoms of cholera include acute profuse, painless watery diarrhoea (rice water stools) of sudden onset, with or without vomiting.
It may be associated with nausea, profuse vomiting, and fever. Severe cases can lead to death within hours due to dehydration (massive body fluid loss). However, most infected people (about 80 per cent) may only show mild symptoms or have no symptoms at all.
The agency noted that people most at risk of cholera are people of all ages living in places with limited access to clean water, people living in areas with poor sanitation and poor hygiene.
It said people living in slum areas where basic water or sanitation infrastructure is missing, people living in rural areas who depend on surface water or unsafe piped or borehole well water sources for drinking, are also at risk.
Others are people who do not perform hand hygiene at appropriate times, man-made or natural disasters like floods resulting in population movements and overcrowded refugee camps, relatives who care for sick people with cholera at home, healthcare workers including doctors, nurses, and other health workers who provide direct patient care in the absence of standard precautions.
Preventive methods
The NCDC emphasized that cholera prevention hinges on ensuring access to safe, potable drinking water, proper sanitation, and waste disposal, alongside maintaining appropriate hygiene practices, such as regular handwashing.
To mitigate the risk of cholera, the NCDC advised the public to boil water and store it in clean, covered containers before drinking. Practicing good personal hygiene, such as frequent handwashing with soap under running water, or using alcohol-based hand sanitizers when soap and water are unavailable, is also crucial.
The NCDC also recommended that food be thoroughly cooked before consumption and protected from contamination by flies and unsanitary handling.
Healthcare workers are also advised to adhere to standard safety precautions and intensify surveillance efforts to promptly report suspected cholera cases.
Additionally, the NCDC urged state governments to prioritize actions that ensure access to and the use of safe water, basic sanitation, and proper hygiene practices in communities.
“As the NCDC continues to work with partners to lead the health sector response to cholera outbreaks, we call for an urgent improvement in access to clean water, proper sanitation, and hygiene,” the statement said.