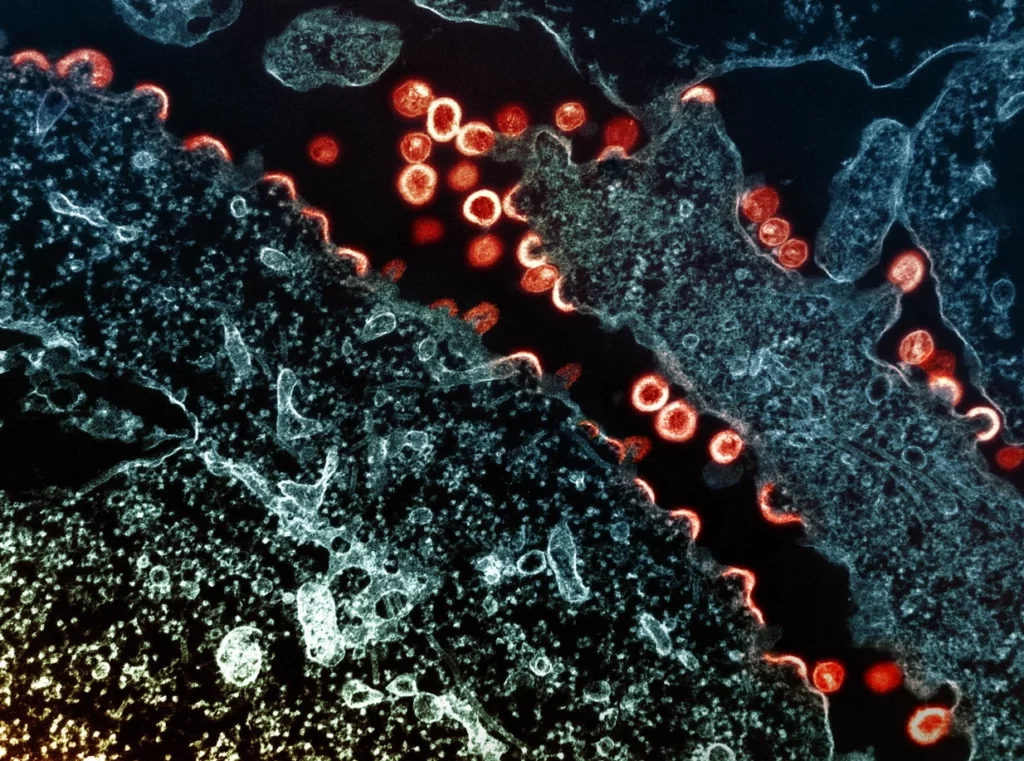
Approximately 39 million people worldwide are living with HIV infection, and while current treatments have been successful in reducing the virus to near undetectable levels, a new study sheds light on a persistent challenge that HIV patients face.
Researchers have discovered that HIV reservoir cells, which remain dormant during treatment, can exist in various body tissues, including the brain. This finding may have significant implications for developing new treatments and understanding the elusive nature of these cells.
For individuals living with HIV, antiretroviral therapy has been a lifeline, helping manage the virus and allowing them to lead relatively healthy lives. However, the virus does not get completely eliminated from the body. Instead, it hides in a reservoir of infected cells, which can become active if treatment is discontinued, leading to a resurgence of the virus and its associated symptoms. This necessitates a lifetime commitment to treatment for those living with HIV.
These HIV reservoir cells often do not express viral proteins, making them challenging for the immune system to detect and eliminate. Furthermore, many of these cells are located in the lymph nodes, which are difficult for researchers to access for study.
To delve deeper into the location and behavior of HIV reservoir cells, a recent study conducted by Sun et al. utilized single HIV genome sequencing. The research team focused on identifying HIV genetic sequences in various body tissues, including the brain, from three individuals who had recently passed away and had agreed to donate their tissues for postmortem studies. Importantly, all three individuals had received antiretroviral therapy until their demise.
The experiments conducted by Sun et al. revealed functional HIV genetic sequences in lymph nodes and gastrointestinal tissues, both of which are known hotspots for HIV-infected cells. More notably, the researchers found genetically intact HIV in the brain tissue of two of the deceased individuals. Strikingly, the HIV genetic sequences in the brain were identical to those found in other body tissues, suggesting that HIV-infected cells had replicated and dispersed throughout the body.
This breakthrough discovery suggests that cells harboring intact HIV are capable of invading the brain and persisting there for extended periods even during antiretroviral therapy. To effectively eradicate the virus, interventions targeting HIV reservoir cells must be capable of reaching the brain.
This new knowledge may assist researchers in developing HIV-reservoir targeting drugs by helping them identify the most promising candidates. Furthermore, future studies may offer insights into the mechanisms that allow HIV to infiltrate the brain and how infected cells manage to evade destruction by the immune system, potentially leading to new treatment strategies.
This study underscores the complex and dynamic nature of HIV within the body and highlights the need for continued research to develop more effective therapies and ultimately move closer to a world without HIV.